Forum on Global Health Ethics Webinar 11: MPOX, Bioethics, and the LGBTQI+
A comprehensive summary of the Forum for Global Health Ethics event held at the University of Zurich on LGBTQI+ stigmatisation and health inequality.
Introduction
In November 2022, the Forum for Global Health Ethics held an online event to discuss LGBTQI+ stigmatisation, the broader issues of health inequality, and bioethics in the wake of the monkeypox (MPOX) outbreak. The forum is an outreach project organised by the Institute of Biomedical Ethics and History of Medicine at the University of Zurich (a World Health Organisation Collaborating Centre for Bioethics). The Forum for Global Health Ethics and the Swiss Medical Weekly jointly organise a webinar series.
Beyond the direct impacts of MPOX on the LGBTQI+ community, the speakers each presented a main concern of the global health response to epidemics, relating to logistical and coordination challenges as well as questions around discrimination and health communication more generally. These key issues touched upon stigmatisation, historic distrust within marginalised communities, and, normatively, how actors should contribute to the policy response alongside communities and authorities.
The webinar was hosted by Nikola Biller-Andorno and Tania Manríquez Roa (University of Zurich, Switzerland). The international experts were Cleiton Euzébio de Lima (Joint United Nations Programme on HIV/AIDS), Julian März (University of Zurich, Switzerland), Stephen Molldrem (University of Texas Medical Branch, United States), and Carla Saenz (Pan-American Health Organisation, PAHO).
Current situation of the MPOX outbreak and inequalities
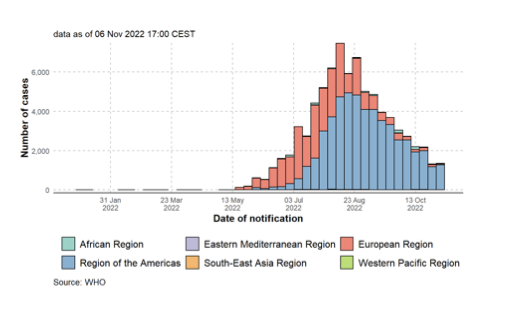
As Cleiton Euzébio de Lima underlined MPOX-V has had a huge influence on the current health situation. There are more than 77,000 confirmed cases and 36 deaths reported regarding MPOX in 109 countries (accessed Oct 27, 2022). In the earlier stages of the outbreak, the worldwide focus on MPOX was mainly on the WHO Europe region, but has now shifted to the WHO Americas region. As seen in Figure 2, a higher proportion of cases were recorded in the Region of the Americas relative to the number of cases recorded in the European Region.
If we look at the people, who have been diagnosed with MPX and gave information about their sexual orientation, over 87% identified themselves as gay, bisexual and other men who have sex with men (MSM). Additionally, the most commonly reported exposure was in a party setting with sexual contact (approximately 43% of the reported exposure settings). Added to this, we have a high rate of co-infections (approx. 49%) with the Human Immunodeficiency Virus (HIV).
Inequities exist both at the national level, along the lines of ethnicity and sexuality (according to CDC data presented by Stephen Molldrem, African Americans and Latinos are overrepresented in the proportion of new MPOX cases), as well as the global level, with regards to focus on the Global North despite the needs of the Global South.
Lessons from the past and the importance of patient experiences
Cleiton Euzébio de Lima focused on lessons from the HIV/AIDS response, making clear that existing prejudices and stigma regarding the LGBTQI+ Community members are impacting the patients in multiple ways. For example, stigma can force people with symptoms to hide their signs of illness instead of visiting a doctor and get medical advice. Therefore, Euzébio de Lima suggests a human right approach to support policy makers in creating laws and policies which empower and protect patients.
To gain such important insights in the patients’ life, emotions and thoughts during the MPOX outbreak, Julian März introduced the DIPEx (“Database of Individual Patients’ Experiences”) project. The DIPEx Methodology is an internationally-vetted method for rigorously and systematically eliciting, analysing, and disseminating maximally heterogeneous health and healthcare experiences.
Ethical challenges in policy-making
A central point of discussion was also how bioethics could and should be integrated into policy-making in response to outbreaks. Julian März highlighted two major themes: firstly ethical considerations regarding health communication (naming, language issues, social context adaptation) and secondly access to healthcare (stigma-free pathways to vaccination and diagnostics).
Carla Saenz underlined the duty of different actors to ensure that inequities and discriminatory practices are not exacerbated by the health response. Communicating ethically is a moral duty that provides a space for public health ethics vocabulary that is distinct from legal and medical language.
Q&A and conclusion
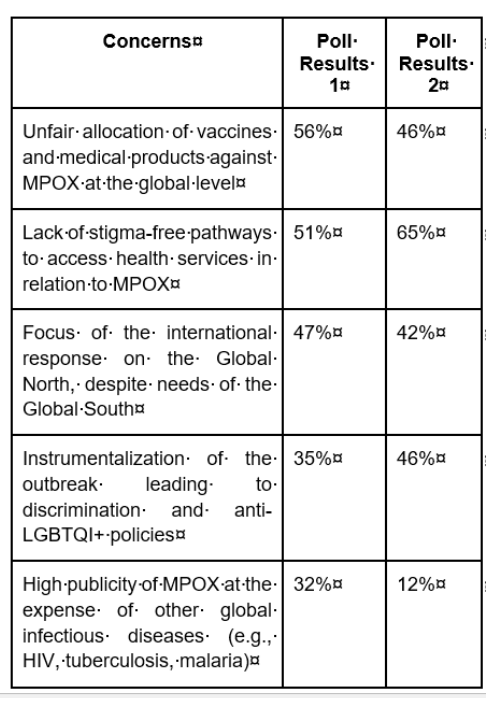
The discussion and Q&A that followed echoed the concerns presented by the expert panel:
- Dealing with challenging legal environments where homosexuality is criminalised requires working with community allies to build responses that do not cause further harm.
- Trust and collaboration must be fostered, keeping in mind ethical guidelines even in technical discussions (e.g., WHO Ethics Guidelines on Public Health Surveillance).
- Each actor at various levels has a responsibility to address challenges to general welfare and society.
Although it is important not to equate the epidemiologies of different outbreaks, whether it is HIV, COVID-19, or MPOX, at each instance there is an opportunity and need to learn from errors in terms of communication, policy formulation, and discourse.